The monetary toxicity of most cancers is rising. That is how we scale back it
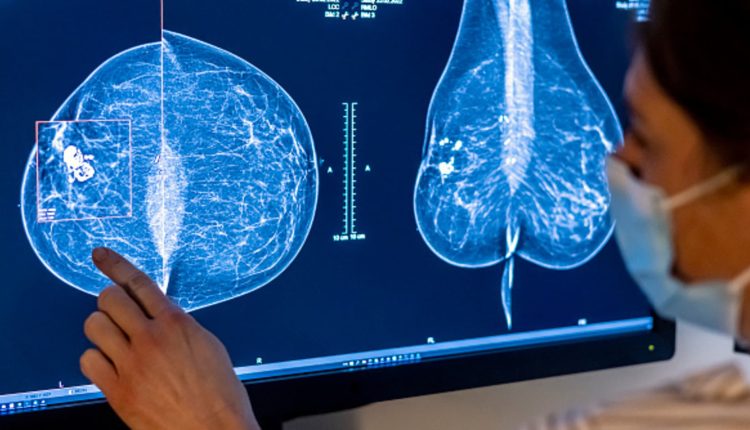
Medical staff uses a mammogram to check a woman's breast for breast cancer.
Hannibal Hanschke | dpa | Picture Alliance | Getty Images
Cancer affects an individual's physical, emotional and financial health. Given the impact on patients and the people in their lives – including their employers – it is time for CEOs to take note and take action to reduce the burden of cancer.
In a study by the American Cancer Society's Cancer Action Network, nearly half of cancer patients and survivors reported being extremely burdened by medical debt. Many respondents had a negative impact of at least $5,000 from their cancer treatment over a period of more than a year, and 42% of cancer patients use up their life savings within the first two years of diagnosis.
Financial hardship caused by cancer can also contribute to “financial toxicity,” where the cost of treatment forces individuals to make compromises that impact their chances of survival. These may include non-biological factors, such as skipping or halving cancer medications to expand supplies, or the inability to complete cancer treatment as planned because of the high cost of transportation to or lodging near cancer treatment centers. This model is unsustainable, and rising costs for new, life-saving cancer treatments will create additional financial burdens – and pose an ever-increasing threat to patients' lives.
The financial toxicity of cancer treatment not only impacts the individual, but can also negatively impact employers. As providers of health insurance to nearly half of the country, employers and unions bear much of the financial burden of cancer. Today, cancer is the largest healthcare cost for medium and large organizations in the United States, and the burden is increasing.
For the first time in history, more than 2 million Americans will receive a new cancer diagnosis in 2024. While the increasing incidence of cancer is partly due to our aging population (the risk of cancer increases with age), we are also seeing a disturbing national trend of younger people being diagnosed with 17 serious cancers. These are people who would likely still be working and using employer-sponsored health insurance. This leaves employers wondering what they can do to reduce the burden of cancer on their population – and their bottom line.
Patients, families and employers all “win” when cancers are diagnosed at an early stage. Early detection of cancer not only improves the chances of survival but also significantly reduces treatment costs. Overall, the cost of treatment for someone diagnosed at stage IV — when the cancer has spread throughout the body — is an average of $156,000 higher than for someone diagnosed at stage I, when the disease is localized. The first year of treatment for colorectal cancer, which affects over 150,000 people in the United States each year and is increasing in younger populations, costs an average of $111,000 when diagnosed at Stage I, with a 5-year survival rate of about 90 % . In contrast, stage IV colon cancer has an average first-year treatment cost of $256,000, and the five-year survival rate is less than 20%. There is evidence that cancer mortality rates would decrease by 30 to 50% if only individuals could take advantage of the prevention, early detection, and cancer treatment strategies that exist today.
These statistics are sound and strongly suggest that concerted efforts by employers and individuals to promote cancer prevention and early detection would improve health and reduce healthcare costs. Today, screening is our best tool for achieving this. Adhering to recommended screening guidelines—such as those published by the ACS—could save the U.S. health care system $26 billion annually in avoided treatment costs.
Despite the importance of early detection and the proven benefits of screening, access to prevention remains a barrier to improved outcomes. Currently, a staggering 65% of eligible Americans have not received recommended cancer screenings. In 2020 alone, Covid-19 restrictions delayed or prevented 9.4 million cancer screenings, likely leading to later diagnoses that would normally have been detected earlier.
There are also logistical and societal hurdles that contribute to financial burdens and impact a person's ability to get screened. In order to attend a screening appointment, people may need to take time off work or arrange childcare. They may need to weigh potential future medical costs against their rent payment obligations. Some may not be aware that they are eligible for screening, and stigma and fear surrounding cancer screening prevent some people from seeking medical care. Inequalities based on socioeconomic status—including place of residence, income, education level, access to health care and healthy foods, and other social determinants of health—create barriers to prevention. To realize the benefits of early detection for individuals and organizations, it is important that we develop new strategies to address these barriers.
Karen Knudsen, CEO of the American Cancer Society
NYSE
ACS is committed to fighting cancer and tackling the challenge of improving access to health care and reducing financial toxicity from multiple perspectives. Similar or supportive actions by U.S. employers will increase our collective contribution to combating the burden of cancer.
With the goal of improving early detection, ACS recently partnered with Color Health in a joint venture to increase employers' and unions' access to screening and preventive care. By making it easier and more convenient for employees to access care – with at-home testing kits and care navigation support throughout their cancer journey – this program aims to increase awareness, accessibility and affordability of cancer screening and early detection. Notably, organizations using the ACS Color program saw a 77% increase in cancer screening compliance.
In addition to direct screening initiatives, programs such as Road to Recovery and ACS Hope Lodges remove the cost burden of transportation and lodging for cancer treatment. Additional partnerships through BrightEdge, the donor-funded innovation and investment arm of ACS, provide access to a broad range of solutions to help people address the financial complexities of cancer across the continuum of care. TailorMed, a portfolio company of BrightEdge, provides a platform that helps patients find resources to cover treatment costs and reduce out-of-pocket costs. Further investments aim to bring the patient voice into therapy and diagnostic development to enable a future generation of sustainable cancer innovations that reduce patient financial hardship.
Advocacy is also key to reducing financial toxicity. ACS's Cancer Action Network advocates for expanding Medicaid to increase access to screening and care for currently uninsured individuals. To reduce prescription drug costs, ACS CAN has also successfully advocated for “smoothing,” a policy that allows Medicare enrollees to spread their prescription drug costs throughout the year. By making payments more manageable for patients, we are eliminating a critical element of the financial challenge of cancer.
One in two women and one in three men will be affected by cancer at some point in their lives. By facilitating guidance-recommended screenings and activating programs that make early detection affordable and accessible, employers can offset financial burdens and improve outcomes for people across the country. When employers help their employees get screenings, they bring us one step closer to eradicating cancer – and its costs – as we know it.
– By Karen Knudsen, CEO of the American Cancer Society (ACS) and the American Cancer Society Cancer Action Network (ACS CAN). She is also a member of the CNBC CEO Council.

Comments are closed.