6 Issues You Ought to Know Earlier than The FDA Panel Votes Immediately
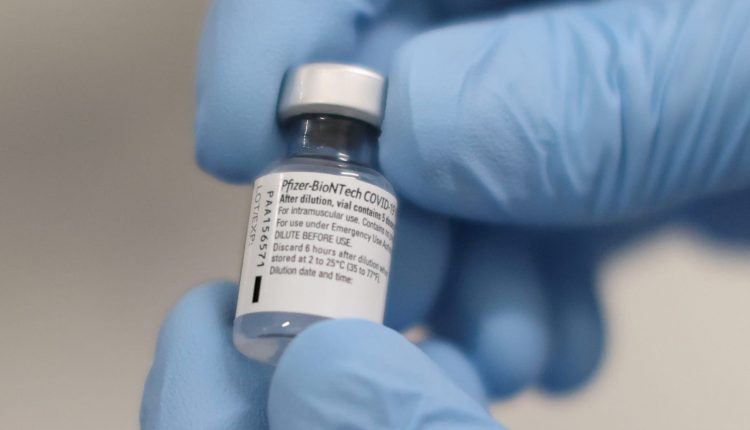
A vial of the Pfizer / BioNTech COVID-19 vaccine.
Liam McBurney | Reuters
A Food and Drug Administration panel is due to vote Thursday on whether to recommend Pfizer and BioNTech’s emergency approval of the coronavirus vaccine.
The non-binding decision of the Agency’s Advisory Committee on Vaccines and Related Biological Products, an external panel of experts on infectious diseases and vaccines, is the final step before the FDA is likely to give final OK on the distribution of the potentially life-saving doses in the United States.
While the FDA may not have to follow the advisory board’s recommendation, the agency often takes its advice. The emergency clearance would mark a pivotal moment in the Covid-19 pandemic that infected more than 15.3 million Americans and killed at least 288,000 people on Wednesday, according to Johns Hopkins University. Hospitals in the U.S. already have higher numbers of Covid patients than ever before, and the country’s outbreak is poised to break even grimmer records.
Pfizer’s vaccine would be the first to be approved for use in the United States
Here’s what you can expect:
1.) When do you vote?
The FDA advisory meeting is scheduled to take place from 9:00 a.m. to 6:00 p.m. The vote is expected to take place towards the end of the meeting. Prior to voting, outside medical experts will evaluate the Pfizer clinical trial data and provide their opinion on the vaccine, including whether the benefits outweigh the risks of being approved for emergency use.
Such approval means that the FDA will allow some people to receive the vaccine as the agency continues to analyze data. This is not the same as a full approval, which can typically take months. To date, Pfizer has only submitted safety data for two months, but it typically takes the agency six months for full approval.
The advisory committee, which is expected to have 23 members, has already reviewed documents submitted by the FDA regarding the Pfizer vaccine, said Dr. Paul Offit, a voting member of the committee. These documents were made available to the public on Tuesday. “The public will see everything we see,” added Offit.
2.) What happens next?
The FDA will make a decision on whether to approve the vaccine for the emergency, which could be given on Friday, committee member James Hildreth told NBC’s Weekend Today on Saturday. Health and Human Services Minister Alex Azar told ABC News “This Week” Sunday that approval could come “within days” of the meeting.
The committee’s recommendation is non-binding, which means that the agency does not have to accept it. But it often does. FDA Commissioner Stephen Hahn said in September that he had “no intention” to override professional scientists at the agency, including Peter Marks, who heads the division that oversees vaccine approvals. “I have full and absolute confidence in the FDA scientists and the decision-making that they have here,” he said on September 10th.
3.) When will the vaccine be distributed?
The federal government is expected to ship 2.9 million doses of Pfizer’s vaccine to jurisdictions across the country within 24 hours of FDA approval for the emergency. This was announced by General Gustave Perna, Chief Operations Officer of Operation Warp Speed, at a briefing on Wednesday.
Another 2.9 million doses are due to be distributed 21 days later for the second dose, he added.
The states had presented the Centers for Disease Control and Prevention with plans early on how they would vaccinate around 331 million Americans against Covid-19 after a vaccine was approved. The CDC has allocated US $ 200 million to the jurisdictions for vaccine preparation, although much of that funding has not reached the local level.
4.) When will I get the vaccine?
The initial doses of the vaccine will be limited as production increases. Officials predict it will be months before everyone in the US who wants to be vaccinated is vaccinated. The vaccine is expected to be distributed in phases, with the CDC urging states to prioritize healthcare workers and nursing homes first.
Dr. Moncef Slaoui, who heads President Donald Trump’s Operation Warp Speed vaccination program, said the US should be able to distribute enough vaccine doses to immunize 100 million Americans, nearly a third of the US population, by the end of February. He said the entire US population could be vaccinated against Covid-19 by June.
5.) Should I get the vaccine if I have Covid?
The FDA said Tuesday that patients who have had Covid-19 may still be at risk of re-infection and could benefit from the vaccine.
The World Health Organization said last week that researchers are still trying to determine how long an antibody response lasts after someone becomes infected with the virus. In a recent study at Oxford, researchers found that it is “highly unlikely” that people who contracted the coronavirus will get the disease again for at least six months.
“We have seen the number of people infected keep growing, but we are also seeing data that protection may not be lifelong and therefore new infections can occur,” said Dr. Mike Ryan, WHO executive director for emergency health program, said Dec. 4. “So the question is: what is the level of protection in society?”
6.) What about side effects?
Most people don’t have serious side effects from vaccines, and serious reactions are extremely rare, according to the Department of Health and Human Services. Pfizer and Moderna vaccines are safe, Slaoui says. Only 10% to 15% of the volunteers report side effects that were “clearly noticeable”.
Participants in Moderna and Pfizer’s coronavirus vaccine trials told CNBC in September that they had a high fever, body pain, severe headache, daytime exhaustion, and other symptoms after receiving the shots. While the symptoms were uncomfortable and at times intense, participants said that they often went away after a day, sometimes sooner, and that it was better than getting Covid-19.
The FDA notes that there is currently insufficient data to draw any conclusions about the safety of the vaccine in children under the age of 16, pregnant women, and people with compromised immune systems.
The UK Medicines Agency warned Wednesday that people with a history of “significant” allergic reactions should not receive the coronavirus vaccine developed by Pfizer.

Comments are closed.